Blog /
Face /
Facial Palsy (Facial Nerve Paralysis): Causes, Symptoms and Treatments
Facial Palsy (Facial Nerve Paralysis): Causes, Symptoms and Treatments
Facial palsy, also known as facial nerve paralysis, occurs when the nerve that controls the facial muscles is damaged or inflamed, leading to weakness or drooping on one side of the face.
It’s more common than many people realise, affecting everyday expressions, eating, and even eye protection. Understanding the causes, symptoms, and recovery options of facial palsy can make a significant difference in effective management.
What Is Facial Palsy (Facial Nerve Paralysis)?
Facial nerve paralysis occurs when the facial nerve (also known as the seventh cranial nerve) becomes inflamed, damaged, or disrupted. This nerve controls the muscles responsible for facial expressions, blinking, and eyelid closure. It also plays a role in tear production and taste sensation.
When the facial nerve doesn’t function properly, the muscles it controls become weak or paralysed. This results in asymmetrical face, difficulty moving facial muscles, and problems with ocular protection.
Facial palsy can affect:
- One side of the face (most common)
- Rarely, both sides
- People of all ages, including children
The severity can range from mild weakness to complete paralysis.
Facial Palsy Causes: Why Does It Happen?
Facial palsy causes come in many forms, from quick hits like viruses to slower builds like tumors, and sorting them out early guides treatment.
- Viral triggers lead the pack: Bell’s palsy, the most common, often stems from herpes simplex or other viruses swelling the facial nerve inside your skull. No one knows exactly why it flares, but cold sores or stress might play a role no clear prevention, just quick steroids to ease swelling.
- Infections beyond viruses: Lyme disease from tick bites, Ramsay Hunt syndrome with shingles rash in the ear, or middle ear infections can spread inflammation to the nerve. Kids might get it from birth-related issues or otitis media gone wrong.
- Trauma and injuries: Car crashes, skull fractures, or even deep cuts to the face can sever or stretch the nerve. Surgical mishaps during parotid gland removal or dental work are always a risk in high-impact spots.
- Tumours and growths: Benign schwannomas or malignant parotid tumours slowly press on the nerve, causing gradual facial asymmetry and facial palsy. Strokes or conditions like sarcoidosis and Guillain-Barré mess with nerve signals too.
- Rare autoimmune or congenital factors: Diabetes ramps up risk by impairing nerve health, while pregnancy hormones spike Bell’s cases in the third trimester. Kids born with Moebius syndrome face lifelong challenges.
Facial Palsy Symptoms: What You Might Notice
Facial palsy symptoms can vary depending on the extent of nerve involvement. Some people notice subtle changes, while others experience sudden and dramatic weakness.
Common symptoms include:
- Drooping of one side of the face
- Difficulty smiling or raising the eyebrow
- Facial asymmetry facial palsy, especially when speaking or laughing
- Changes in speech clarity
- Drooling from one side of the mouth
- Altered taste sensation
- Sensitivity to sound in one ear
For many patients, the most uncomfortable and concerning symptoms involve the eyes.
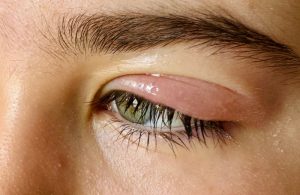
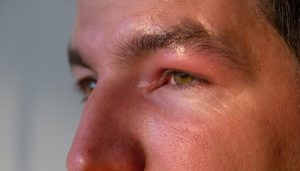
Facial Palsy Eye Problems: Why the Eyes Are So Affected
Eye involvement is one of the most challenging aspects of facial palsy. The facial nerve controls blinking and eyelid closure, both of which are essential for maintaining ocular moisture and protection.

Ready to achieve your aesthetic goals?
- Over a Decade of Surgical & Aesthetic Expertise
- Personalised treatment plans tailored to your needs
Common Eye Issues in Facial Palsy
- Inability to close eye due to facial palsy
When the eyelid muscles weaken, blinking may become incomplete or cease altogether.
- Lagophthalmos facial palsy
This term describes incomplete eyelid closure. Even a small gap can lead to dryness and irritation.
- Dry eye facial palsy
Without proper blinking, tears don’t spread evenly across the eye, leading to dryness, burning, and discomfort.
- Eye exposure facial palsy
The exposed surface of the eye becomes vulnerable to wind, dust, and injury.
- Facial palsy eye problems can worsen at night when the eye remains partially open during sleep, increasing the risk of corneal damage.
Treatment Options for Facial Palsy (Facial Nerve Paralysis)
Treatment for facial nerve paralysis focuses on protecting the eye, supporting nerve recovery, improving facial balance, and helping patients regain comfort and confidence. There is no single treatment that works for everyone, and care is usually tailored based on the cause, severity, and stage of facial palsy.
1. Early Medical Treatment
In the early stages, particularly in cases such as Bell’s palsy, prompt medical care can facilitate recovery.
- Corticosteroids are often prescribed to reduce inflammation around the facial nerve.
- Antiviral medication may be added if a viral cause is suspected
- Pain relief may be used if there is discomfort around the ear or jaw
Early treatment can improve the likelihood of recovery from facial palsy, particularly when initiated within the first few days.
2. Eye Protection and Eye Care (Most Important)
Eye care is a priority in facial palsy because weakness of the eyelid muscles can lead to exposure and dryness.
Common eye-focused treatments include:
- Artificial tears during the day
- Lubricating ointments at night
- Moisture goggles or eye taping while sleeping
- Protective glasses outdoors
These measures help manage dry eye and facial palsy and reduce the risk of corneal damage caused by lagophthalmos or the inability to close the eye due to facial palsy.
3. Facial Physiotherapy and Exercises
Facial physiotherapy helps maintain muscle tone and coordination as the nerve heals.
- Gentle facial exercises guided by a specialist
- Massage techniques to reduce stiffness
- Neuromuscular retraining in later stages
This approach supports symmetry and may reduce long-term facial asymmetry and facial palsy.
4. Management of Eyelid Drooping and Asymmetry
As facial palsy stabilises, some patients continue to experience:
- Eyelid drooping facial palsy
- Drooping eyelid facial palsy
- Eyelid asymmetry
In selected cases, procedures may be considered to improve eyelid position and eye protection.
Role of Blepharoplasty (Supportive, Not Curative)
It’s important to be clear:
- Blepharoplasty does not treat facial palsy
- It does not repair the facial nerve
However, blepharoplasty may help manage eyelid problems caused by facial palsy by:
- Improving eyelid position
- Reducing eyelid heaviness
- Improving eyelid symmetry
- Supporting better eye protection
This option is considered only after careful evaluation and typically once facial palsy has stabilised.
5. Non-Surgical Eyelid Support Options
Before considering any procedure, doctors may recommend:
- Eyelid taping techniques
- External eyelid weights
- Temporary measures to improve blinking and closure
These can be helpful for patients with ongoing facial palsy eye problems.
6. Long-Term Support and Monitoring
Facial palsy recovery takes time. Some patients recover fully, while others may have residual symptoms that need ongoing care.

Ready to achieve your aesthetic goals?
- Over a Decade of Surgical & Aesthetic Expertise
- Personalised treatment plans tailored to your needs
Long-term management may include:
- Regular eye checkups
- Continued lubrication for dry eye
- Adjustments in treatment as nerve function changes
- Emotional and psychological support
7. When to Seek Specialist Care
You should seek specialist assessment if you experience:
- Persistent inability to close eye facial palsy
- Worsening dry eye and facial palsy
- Vision changes or eye discomfort
- Ongoing eyelid drooping and facial palsy affecting daily life
Early and appropriate care helps protect vision and improves overall comfort.
Practical Daily Tips for Recovery
Smooth days amid facial palsy-related eye problems come from smart habits that blend protection, exercise, and mindset.
- Eye defense kit:
- Sunglasses wraparounds cut glare from eye exposure to facial palsy.
- A humidifier at home mitigates dry air, which can exacerbate dry eye and facial palsy.
- Meal and speech hacks:
- Straws and soft foods are recommended to prevent drooling in cases of facial asymmetry or facial palsy.
- Chew the opposite side, and practice vowels loudly.
- Exercise lineup (10 mins daily):
- Raise brows, hold 5 sec.
- Pucker lips, smile wide alternately.
- Blink squeezes for lagophthalmos facial palsy.
- Lifestyle boosts:
- Avoid irritants like smoke; manage stress with walks.
- Support groups share coping narratives about eyelid asymmetry.
- Warning trackers:
- Log symptoms daily; alert doc if worsening.
Final Thoughts
Living with facial palsy or facial nerve paralysis doesn’t have to define your days. Many people bounce back strong with the right mix of early care, eye protection, and steady rehab to tackle facial palsy eye problems like lagophthalmos, dry eye, and eyelid drooping.
From identifying the causes and symptoms of facial palsy to progressing through recovery, the key is consistent steps that safeguard vision, ease asymmetrical face, and restore confidence in everyday moments. Whether it’s drops for inability to close the eye, facial palsy, therapy for eyelid asymmetry, or specialist interventions, proactive management turns challenges into manageable parts of life, allowing you to focus on what matters most.
FAQs
01. What are the most common causes of facial palsy in 2025?
Viral infections like Bell’s palsy still lead, but rising Lyme disease cases from outdoor activities and post-COVID nerve issues are trending higher this year.
02. How long does facial palsy recovery typically take now?
Most see major gains in 3-6 months with steroids and therapy, but new e-stim devices are speeding things up for stubborn facial asymmetry and facial palsy cases.
03. Can dry eye facial palsy lead to serious vision loss?
Yes, untreated eye exposure, facial palsies, and lagophthalmos increase the risk of corneal ulceration, prompting recommendations for nightly ointment and moisture shields.
04. What’s the best fix for the inability to close the eyelid in facial palsy?
Gold weight implants or taping are effective in the short term; blepharoplasty may help manage eyelid problems caused by facial palsy, improving position and protection in select cases.
05. How to reduce eyelid drooping and facial palsy at home?
Daily lid massages, warm compresses, and blink exercises help; emerging TikTok tips pair them with hyaluronic drops for rapid relief from drooping eyelids in facial palsy.