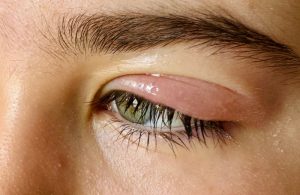
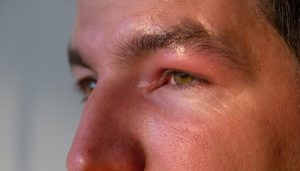
Have you ever glanced in the mirror and noticed a new bump, rash, or spot on your skin that just doesn’t look right? You’re not alone. Skin lesions pop up on millions of people every year, sometimes harmless, sometimes signalling something more serious.
Understanding types of skin lesions can help you stay on top of your skin health and know when it’s time to chat with a pro. In this blog, we will explore skin lesion types. We’ll break it all down with real talk, pictures in mind (check out our skin lesion types chart later), and tips straight from dermatology experts.
What are Skin Lesions?
Skin lesions are basically any change in your skin’s colour, texture, or thickness compared to the area around it. They can be tiny freckle-like spots or larger patches that itch or hurt. The good news? Most are treatable, especially if caught early at a place like our clinic, where we specialise in personalised skin checks.
Let’s get into the details so you feel confident spotting and handling them.

Primary Skin Lesions: The Starting Point
Primary skin lesions are the original ones that appear first, without any scratching or irritation, and do not turn into something else. Think of them as the skin’s first “hey, something’s up” signal. Doctors use specific terms to describe them based on size, shape, and feel; it’s like learning a secret language for your dermatology visits.
- Macules: Flat, discoloured spots less than 1 cm across, like freckles or the flat parts of vitiligo. They’re not raised or bumpy, just a colour change that blends into normal skin edges. Common in sun-exposed areas.
- Papules: Small, solid, raised bumps under 1 cm, often from acne or warts. Feel them with your fingers; they’re firm, not squishy. Psoriasis can start this way, too.
- Nodules: Like papules but bigger (over 1 cm) and deeper, such as cysts or certain tumours. They might feel hard under the skin and stick around longer.
- Vesicles and Bullae: Fluid-filled blisters. Vesicles are small (under 1 cm), like those from poison ivy; bullae are larger and seen in burns or severe allergic reactions. They can burst and ooze.
- Pustules: Pus-filled bumps, think acne pimples or folliculitis. Yellowish-white centres make them stand out.
- Plaques: Raised, flat-topped lesions larger than 1 cm that often form when papules merge together. Plaques are commonly seen in conditions like psoriasis, chronic eczema, and lichen planus, and they may feel thick or scaly to the touch.
- Wheals (Hives): Soft, raised, itchy lesions that appear suddenly and usually disappear within hours. Wheals are commonly caused by allergic reactions, food sensitivities, medications, or stress-related urticaria.
- Cysts: Closed, sac-like lesions filled with fluid or semi-solid material. Epidermoid and sebaceous cysts are common examples and often feel smooth, movable, and slow-growing beneath the skin.
These types of skin lesions are often tied to infections, allergies, or genetics. For example, moles are classic primary lesions that most of us have, but changes in size or colour warrant a closer look.
Secondary Skin Lesions: What Happens When Things Evolve
Once a primary lesion is irritated, say, by scratching or rubbing, it can morph into a secondary lesion. This is your skin’s way of healing (or reacting), but it can make diagnosis trickier. Knowing the types of skin lesions at this stage helps doctors pinpoint causes faster.
Common secondary skin lesions include:
- Scales: Flaky, dry bits peeling off, like in eczema or psoriasis. They build up from dead skin cells.
- Crusts: Dried fluid or blood forming a scab post-blister or infection. Honey-coloured crusts scream impetigo.
- Erosions: Shallow skin loss without scarring, from popped vesicles. They heal quicker than ulcers.
- Ulcers: Deeper craters eating into skin layers, often from poor circulation or pressure sores. Painful and slow-healing.
- Scars and Atrophy: Thickened keloids or thinned, wrinkled skin after injury. Keloids grow beyond the original wound.
- Fissures: Deep cracks in thickened or very dry skin, commonly seen on heels, fingertips, or lips, especially in eczema, fungal infections, or diabetes.
- Lichenification: Thickened skin with exaggerated skin lines caused by chronic scratching or rubbing, often associated with long-standing eczema or neurodermatitis.
Secondary lesions remind us why hands-off is best; picking worsens things. At our clinic, we see tons of these from everyday habits like tight clothes or harsh soaps.
Acne and Acne-Related Skin Lesions
Acne is one of the most common causes of skin lesions, particularly in teenagers and adults with hormonal imbalances. Acne-related lesions can vary in depth and severity and may appear on the face, chest, back, or shoulders.

Ready to achieve your aesthetic goals?
- Over a Decade of Surgical & Aesthetic Expertise
- Personalised treatment plans tailored to your needs
- Comedones: Non-inflammatory acne lesions that include blackheads (open comedones) and whiteheads (closed comedones). These occur when pores become clogged with oil and dead skin cells.
- Inflammatory Acne Lesions: Papules and pustules that appear red, swollen, and sometimes painful. These are commonly referred to as pimples.
- Acne Nodules and Cysts: Large, deep, painful lesions that form under the skin and carry a higher risk of scarring if not treated properly.
Early treatment of acne-related skin lesions helps prevent permanent scarring and pigmentation issues.
Moles (Nevi) as Skin Lesions
Moles, medically known as nevi, are common skin lesions formed by clusters of pigment-producing cells. Most people have multiple moles, and they are usually harmless.
- Common (Benign) Moles: Small, round or oval lesions with uniform colour and smooth borders that remain stable over time.
- Congenital Moles: Present at birth and may vary in size. Larger congenital moles require regular monitoring due to a slightly higher cancer risk.
- Atypical (Dysplastic) Moles: Irregular in shape, colour, or size, and may resemble melanoma. These require close dermatological observation.
Any mole that changes in size, shape, colour, or starts bleeding or itching should be evaluated promptly.
Benign Skin Lesions: Usually No Big Worry
Most skin lesions we encounter daily are benign, meaning non-cancerous. They might cause cosmetic irritation or itching, but they’re not life-threatening. Here’s a rundown of frequent flyers:
- Seborrheic Keratoses: Waxy, stuck-on-looking growths, brown or black, common after 40. They feel rough like sandpaper.
- Skin Tags: Tiny, soft flaps in friction spots like neck folds or armpits. Harmless but easy to snip off.
- Cherry Angiomas: Bright red dots from clustered blood vessels, popping up with age. Laser zaps them quick.
- Dermatofibromas: Hard, brownish nodules from insect bites or splinters. Dimple when pinched.
- Actinic Keratoses: Precancerous rough patches from sun damage, often red or scaly on the face/hands. Early treatment prevents worse.
These benign types of skin lesions affect over half of adults by midlife. Sun protection and moisturising cut risks, but removal is straightforward if they’re in the way.
Precancerous and Malignant Skin Lesions: Red Flags
Not all skin lesion types are chill; some signal precancer or cancer. Spotting them early saves skin and peace of mind. Use the ABCDE rule for moles: Asymmetry, irregular borders, varied colour, diameter over 6 mm, evolving changes.
- Actinic Keratoses (AKs): Already mentioned, but they’re the most common precancer. Rough, gritty feel; 10% turn to squamous cell carcinoma if ignored.
- Bowen’s Disease: Red, scaly patch mimicking eczema, but it’s squamous cell carcinoma in situ (surface-only). Slow-growing on legs or trunk.
- Basal Cell Carcinoma (BCC): A pearly bump or sore that won’t heal, often on the face. Slow but locally invasive.
- Squamous Cell Carcinoma (SCC): Scaly red patch or ulcer, faster-growing than BCC, sun-linked.
- Melanoma: A dangerous flat or raised lesion with uneven edges/colours. Check your back hard to see yourself.
Risk increases with fair skin, a history of sun exposure, or family history. Our clinic’s full-body exams catch these early with dermoscopy tools.
Types of Skin Lesions Chart: Quick Visual Reference
For easy recall, here’s a chart of types of skin lesions summarising primaries and secondaries. Print it or save for your next self-check!
| Type | Description | Size | Example Conditions | Image Idea |
|---|
| Macule | Flat, colour change | < 1 cm | Freckle, vitiligo | Flat brown spot |
| Papule | Raised, solid | < 1 cm | Acne, warts | Small red bump |
| Nodule | Raised, solid, deep | > 1 cm | Cyst, lipoma | Firm lump under skin |
| Vesicle | Fluid-filled blister | < 1 cm | Herpes, contact dermatitis | Clear tiny bubble |
| Pustule | Pus-filled | < 1 cm | Impetigo, folliculitis | White-headed pimple |
| Scale | Flaky dry layer | Varies | Psoriasis, dandruff | Peeling white flakes |
| Crust | Dried scab | Varies | Post-blister | Yellowish scab |
| Ulcer | Open sore | Varies | Venous stasis | Deep crater |
Causes Behind Skin Lesions
Skin lesions arise from a mix of everyday exposures and deeper health issues, ranging from simple rashes to worrisome growths. Here’s a breakdown of the top five causes, drawn from common medical insights, to help you spot triggers early.
- Infections: Bacterial (like staph causing impetigo or boils), viral (herpes blisters, shingles, chickenpox), fungal (ringworm patches), or parasitic (scabies burrows) invasions lead to pus-filled pustules, vesicles, or itchy scales, often spreading quickly in warm, moist areas.
- Sun Exposure and UV Damage: Chronic or intense sunlight triggers actinic keratoses (rough precancerous spots), solar lentigines (age spots), or even basal/squamous cell carcinomas, especially on fair skin or after childhood burns.
- Allergic Reactions and Irritants: Contact with allergens (poison ivy, nickel), foods, meds, or harsh products sparks hives, eczema flares, or contact dermatitis, showing as red, itchy macules, plaques, or blisters that evolve into secondary crusts.
- Autoimmune and Chronic Conditions: Disorders such as psoriasis (silvery scales), eczema (dry patches), lupus (butterfly rash), or vitiligo (white macules) cause the immune system to attack the skin, creating persistent skin lesions that worsen with stress or weather.
- Trauma, Injuries, and Medications: Cuts, burns, friction (leading to skin tags or calluses), chemotherapy side effects, or systemic diseases (diabetes, slow-healing ulcers) can cause erosions, scars, or nodules as the skin reacts and repairs.
Treatment Options for Skin Lesions
Topical Medications
Many skin lesions, particularly those caused by inflammation or infections, respond well to topical treatments. These include medicated creams, ointments, and gels that reduce inflammation, control infection, or promote healing.
Common ingredients in these medications include corticosteroids to reduce swelling and redness, antibiotics for bacterial infections, antifungal creams, and keratolytic agents like salicylic acid that help peel off scaly lesions, such as actinic keratosis. Topical treatments such as 5-fluorouracil or imiquimod may be prescribed to destroy abnormal cells.
Cryotherapy
Cryotherapy involves freezing the lesion using liquid nitrogen, which causes the abnormal tissue to die and eventually slough off. This method is effective for treating warts, seborrheic keratoses, actinic keratoses, and some small precancerous or cancerous lesions. It is a quick outpatient procedure and typically leaves minimal scarring.
Laser Therapy
Laser treatment is a non-invasive option that targets specific skin lesions by delivering focused light energy to remove or reduce them. It is often recommended for vascular lesions like cherry angiomas, certain types of scars, birthmarks, and some pigmented lesions. Laser therapy can also be used after a biopsy to refine cosmetic outcomes.
Photodynamic Therapy (PDT)
Photodynamic therapy is a specialised approach that combines a photosensitising topical medication with a specific light source to activate it, killing cancerous or precancerous skin cells. This is commonly used for actinic keratoses and superficial basal cell carcinomas. PDT provides a targeted treatment with minimal damage to surrounding healthy skin.

Ready to achieve your aesthetic goals?
- Over a Decade of Surgical & Aesthetic Expertise
- Personalised treatment plans tailored to your needs
Surgical Removal
Surgical excision remains one of the most effective ways to treat many types of skin lesions, especially malignant or suspicious ones. The lesion is cut out with a margin of healthy tissue to ensure complete removal.
Techniques include shave excision, curettage (scraping), and more precise methods like Mohs micrographic surgery, which is particularly useful for skin cancers on the face or other sensitive areas. Surgery allows for biopsy and histopathological examination as confirmation.
Other Treatments
- Electrocautery or Electrodessication: These involve using heat or electrical current to destroy lesions such as skin tags or superficial warts.
- Oral Medications: In cases of widespread infection or certain chronic skin conditions, oral antibiotics, antivirals, or antifungal drugs might be used.
- Home Remedies: For benign lesions such as warts, some topical salicylic acid products are available for home use, but should be used cautiously.
When to consult a Doctor
Spotting skin lesions early is smart, but certain signs mean it’s time to see a dermatologist right away. Don’t wait for them to worsen. Use the ABCDE rule for moles or growths: Asymmetry (uneven shape), irregular borders, variegated colours, diameter over 6mm, or evolving changes like growth or itching.
Key red flags include:
- Rapid changes: Lesion grows, changes colour/shape, or appears new after age 30.
- Symptoms like pain, itch, or bleeding: Especially if crusting, oozing pus, or not healing in 2-4 weeks.
- Infection signs: Fever, swelling, red streaks, or warmth around the skin lesion could be cellulitis.
- Widespread or stubborn issues: Rash spreads, covers body, or resists home care; hives lasting weeks.
- High-risk factors: Personal/family history of skin cancer, many moles, or sun-damaged skin.
Wrapping Up Skin Lesions
Skin lesions come in many forms, from harmless bumps to serious spots, but knowing the types of skin lesions and their causes empowers you to act fast. Regular self-checks with a types of skin lesions chart, sun protection, and gentle care go a long way in prevention.
Spot changes? Don’t wait for early visits to our clinic to catch issues before they grow. Stay vigilant, protect your skin daily, and enjoy healthier, clearer skin ahead. Your skin tells a story; let’s keep it a good one.
FAQs
1. What are the main types of skin lesions?
Skin lesion types include primary lesions, such as macules (flat spots), papules (raised bumps), and vesicles (blisters), and secondary lesions, such as scales or crusts from irritation. Use a skin lesion chart for visuals.
2. Are all skin lesions cancerous?
No, most skin lesions are benign, like skin tags or seborrheic keratoses. Precancerous (actinic keratoses) or malignant (melanoma) ones show asymmetry, colour changes, or growth get them checked.
3. How can I prevent skin lesions at home?
Daily SPF 30+ moisturiser, avoid irritants, and do monthly self-exams. Clean wounds promptly to avoid infections and the development of skin lesions.
4. When should I see a dermatologist for a skin lesion?
If it’s growing, bleeding, itchy/painful, or changes shape/colour, or lasts over 2 weeks. Our clinic offers quick dermoscopy for peace of mind.
5. What treatments fix most skin lesions?
Topicals (steroids, antifungals), cryotherapy, lasers, or excision work for skin lesion types. Benign ones often need simple removal; cancers get targeted surgery.